Gut Instincts: Why Your Cravings Are Trauma Talking
That 3 AM kitchen raid isn’t about hunger.
The afternoon sugar crash that sends you hunting for candy isn’t weakness.
That overwhelming need for carbs when stressed isn’t lack of discipline.
What’s really happening? Your cravings are your body’s attempt to communicate unmet needs, unprocessed emotions, and unhealed trauma through the only language it knows you’ll listen to: urgent, undeniable physical sensation.
And here’s the key: knowing and listening to this conversation between gut and brain transforms how we approach both healing and eating.
The Gut-Brain Connection
Deep within your digestive system lives what scientists call the “second brain” – the enteric nervous system, containing over 500 million neurons, more than your spinal cord.
This isn’t metaphorical; your gut literally thinks, feels, and remembers independently while maintaining constant communication with your primary brain.
How? The vagus nerve, the longest cranial nerve, acts as a superhighway for bidirectional signals.
This gut-brain axis operates through multiple channels: neural pathways via the vagus nerve, hormonal signals through the bloodstream, immune system mediators, and perhaps most surprisingly, through the trillions of microbes living in your intestines.
These bacteria don’t just help digest food. They produce neurotransmitters like serotonin (90% made in the gut), dopamine, and GABA that directly influence mood, anxiety, and yes, cravings.
When this system is balanced, communication flows smoothly. When trauma disrupts it, the messages become scrambled, urgent, and often manifest as insatiable cravings.
How Trauma Rewires the Gut
Chronic stress and trauma fundamentally alter gut function through the hypothalamic-pituitary-adrenal (HPA) axis.
When your nervous system perceives threat – whether from actual danger or traumatic memories – it diverts resources away from digestion toward survival.
Blood flow decreases, motility changes, intestinal permeability increases (leaky gut), and the delicate balance of gut bacteria shifts toward inflammatory, anxiety-promoting species.
This creates a vicious cycle: trauma disrupts the gut, the disrupted gut sends danger signals back to the brain, the brain interprets these signals as requiring immediate action, and cravings emerge as the fastest solution.
Research shows that people with PTSD have measurably different gut microbiomes than those without trauma, with less diversity and more inflammatory bacteria.
Your environment shapes these microbial communities as much as your diet, with poverty, pollution, and chronic stress all influencing which bacteria thrive.
Dysbiosis: When Bad Bacteria Take Over
Dysbiosis – an imbalance in gut bacteria – doesn’t just affect digestion. It fundamentally alters brain chemistry and behavior.
Harmful bacteria produce compounds that increase inflammation, disrupt the blood-brain barrier, and hijack your reward systems. They literally send signals making you crave the foods they need to survive: sugar, refined carbs, processed foods.
Studies show that certain bacteria can manipulate host eating behavior to increase their own fitness. They release toxins that make us feel bad until we eat what they want, then reward us with dopamine when we comply. It’s biological manipulation at the cellular level.
This explains why sugar cravings can feel so urgent and specific – it’s not just you wanting sweetness, it’s billions of microorganisms demanding their preferred fuel.
Understanding Cravings vs. Emotional Needs – When Hunger Isn’t About Food
Trauma disrupts interoception – your ability to read internal body signals accurately.
When you’ve learned to disconnect from your body for survival, all internal sensations blur together:
- Loneliness feels like hunger
- Anxiety mimics low blood sugar
- Exhaustion registers as needing chocolate
The need for comfort, safety, or connection gets misinterpreted as requiring food because eating is one of the few reliable ways trauma survivors learned to self-soothe.
This confusion isn’t a personal failing – it’s a neurological adaptation. Children who didn’t receive consistent co-regulation and whose emotions weren’t validated or named never developed the neural pathways to distinguish among different internal states.
If no one helped you understand that the pit in your stomach was fear, not hunger, or that the emptiness in your chest was grief for what you never received, not a need for food, then eating becomes the universal solution to all discomfort.
Seeing Food as Reliable Comfort
For many trauma survivors, food was the only consistent source of comfort in an unpredictable world.
Unlike people, food doesn’t judge. It doesn’t abandon you. It doesn’t hurt you.
Plus, it’s available 24/7, provides immediate relief, and requires no vulnerability or trust.
This makes emotional eating not just logical but brilliant – a survival strategy that worked when nothing else did.
The foods we crave during emotional distress aren’t random:
- Sugar provides quick energy when the nervous system is depleted from hypervigilance.
- Carbohydrates boost serotonin when trauma has disrupted natural production.
- Fat satisfies the deep need for nurturing that was missing in childhood.
- Salt helps a dysregulated nervous system maintain basic functions.
These cravings are your body’s attempt to self-medicate with the tools available. A mental health platform that understands this removes shame from the conversation.
The Unmet Needs Behind Cravings
Decoding cravings requires asking what emotional need might be disguised as hunger.
That chocolate craving? It might be loneliness seeking the oxytocin boost chocolate provides. The chips obsession? It could be anger needing something to crunch.
Late-night eating often masks the fear of being alone with thoughts when defenses are down.
Knowing and seeing cravings as communication rather than weakness transforms your relationship with them.
Instead of fighting the craving, you can ask: What am I really hungry for? Touch? Purpose? Safety? Rest?
This doesn’t mean never eating for comfort – sometimes that chocolate is exactly what you need. But awareness creates choice where once there was only compulsion. Social emotional learning includes recognizing these deeper hungers and finding various ways to feed them.
Why It’s Not About Willpower
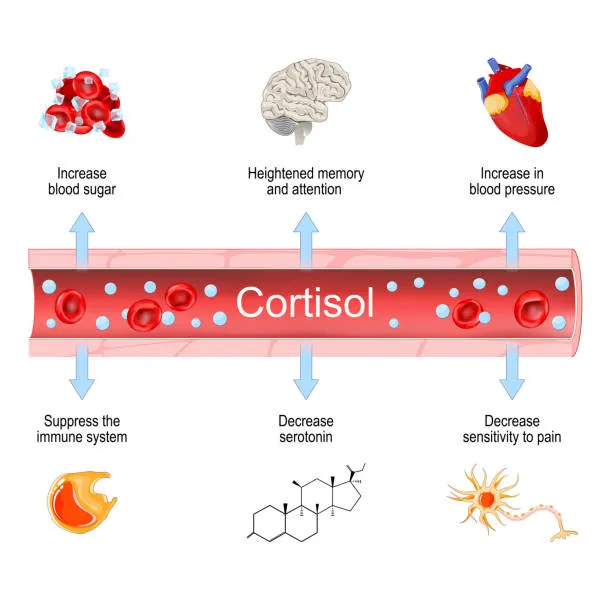
When trauma keeps your nervous system in chronic stress, cortisol remains perpetually elevated.
This stress hormone raises blood sugar to fuel fight-or-flight responses, but when the threat never ends, this system breaks down.
In fact, your body’s cells can become resistant to insulin’s signals. Your blood sugar swings wildly, and your body desperately craves quick energy sources to stabilize.
This biological chaos makes refined carbohydrates and sugar irresistible – not because you’re weak, but because your body is trying to survive what it perceives as ongoing danger.
The resulting blood sugar rollercoaster creates its own stress, triggering more cortisol, worsening insulin resistance, and intensifying cravings. It’s a metabolic manifestation of chronic stress that willpower alone cannot overcome.
Sleep Deprivation’s Hidden Role
Trauma disrupts sleep, and sleep disruption intensifies cravings.
When you don’t get adequate rest, ghrelin (hunger hormone) increases while leptin (satiety hormone) decreases. Your brain, desperate for energy, specifically craves calorie-dense foods high in sugar and fat.
Studies show that sleep-deprived individuals consume an average of 385 extra calories per day, primarily from snack foods.
But it goes deeper than hormones. Sleep deprivation impairs the prefrontal cortex – the brain region responsible for impulse control and decision-making – while heightening activity in reward centers.
This means you simultaneously want food more intensely while having less ability to resist. For trauma survivors already dealing with nervous system dysregulation, sleep loss creates a perfect storm of irresistible cravings.
The Biology of Sugar Addiction
Sugar addiction in trauma survivors isn’t metaphorical. Trauma alters dopamine signaling, requiring more stimulation to achieve the same reward response.
Sugar provides that stimulation, temporarily restoring neurotransmitter balance that trauma disrupted. Brain imaging shows that sugar activates the same reward pathways as addictive drugs, and withdrawal creates similar discomfort.
The food industry exploits this biology, engineering products that hit the “bliss point”—the precise combination of sugar, salt, and fat that overrides satiety signals and triggers compulsive consumption.
For someone whose nervous system is already dysregulated from trauma, these foods aren’t just tempting – they become neurologically irresistible.
The trauma economy profits from keeping us craving what harms us while selling us shame for the cravings they created.
Rewiring with Awareness – It’s Possible
When It’s Time to Pause and Decode
The first step in healing trauma-driven cravings? Creating space between urge and action. When a craving hits, pause for thirty seconds. Not to resist, but to investigate.
Place your hand on your chest or stomach and ask:
- What am I actually feeling right now?
- Am I physically hungry, or is this emotional?
- What happened right before this craving emerged?
This isn’t about judging or stopping the craving. Go ahead and eat the cookie if you need to!
But awareness begins to restore the connection between sensation and meaning that trauma severed.
Over time, you might notice patterns: sugar cravings after criticism, carb binges when lonely, restriction when anxious. These patterns are information, not character flaws, and they reveal how your nervous system learned to cope and point toward what needs healing.
Somatic Tools for the Moment
When you recognize a craving as emotional rather than physical, somatic tools can provide alternative regulation without food. These aren’t replacements for eating. But having options creates flexibility where trauma created rigidity.
Try the HALT check: Am I Hungry, Angry, Lonely, or Tired?
- If hungry, eat mindfully. If angry, try vigorous movement or journaling.
- If lonely, reach out to someone safe or engage with a healthy lifestyle community.
- If tired, rest rather than using sugar for false energy.
These simple interventions honor the need behind the craving while expanding your self-soothing toolkit.
For immediate nervous system regulation, try box breathing (4 counts in, hold 4, out 4, hold 4) to activate your parasympathetic nervous system.
Drink a full glass of water slowly, feeling it move through your body. Step outside and feel sunlight or fresh air on your skin.
These micro-interventions don’t eliminate cravings but reduce their urgency, creating space for conscious choice.
Long-Term Gut Repair
Healing the gut-brain axis requires consistent, gentle interventions rather than dramatic overhauls.
Start by adding diversity to your diet.
This isn’t removing “bad” foods but adding variety to feed beneficial bacteria. Include fermented foods like yogurt, kefir, sauerkraut, or kimchi daily. These provide probiotics that can shift your microbiome toward balance.
Increase prebiotic fiber gradually through vegetables, legumes, and whole grains.
These feed beneficial bacteria and help them produce short-chain fatty acids that reduce inflammation and support mood.
But go slowly – traumatized guts often react strongly to sudden dietary changes. A personal growth platform that includes nutrition guidance can help navigate this process without triggering restriction or binge patterns.
Consider a Mediterranean-style eating pattern, repeatedly shown to support both gut and mental health.
This isn’t a diet but a flexible approach emphasizing whole foods, healthy fats, and diverse plant foods while allowing for pleasure and flexibility. The goal isn’t perfection but gradually supporting your gut’s ability to communicate clearly with your brain.
We Need to See Nervous System Work as the Foundation of Holistic Health
Sustainable craving changes require nervous system regulation. All the dietary changes in the world won’t stick if your body remains in survival mode.
This is why addressing trauma’s impact on your nervous system must accompany any gut healing protocol.
- Vagus nerve stimulation through humming, singing, or gargling can improve gut-brain communication.
- Regular movement helps discharge trapped trauma energy that might otherwise drive cravings.
- Consistent sleep hygiene supports hormone regulation.
These are fundamental to healing the system that generates them.
Most importantly, develop self-compassion for the cravings themselves. They’re not weakness or failure, but your body’s attempt to manage an impossible situation with limited tools.
Every craving is a communication from a part of you that’s trying to help, even if its methods are outdated. Mental health education that frames cravings this way removes shame and creates space for curiosity and healing.
Taking the Next Step Toward Healing Through Awareness
Healing trauma-driven cravings isn’t about developing stronger willpower or finding the perfect diet.
It’s about rebuilding the communication channels between gut and brain that trauma disrupted. It’s learning to speak your body’s language and teaching it that safety is possible.
This journey requires patience. Your gut microbiome took years to develop its current state – it won’t transform overnight.
Your nervous system learned to use food for regulation through thousands of repetitions – it needs time to trust new strategies.
Above all, be gentle with yourself as you navigate this process. Every moment of awareness, every pause before acting on a craving, every kind word to yourself when you struggle—these are victories that accumulate toward lasting change.
Remember that cravings aren’t the enemy. They’re messengers.
When we learn to decode their language, they become guides toward what we really need: safety, connection, rest, play, purpose. The goal isn’t to eliminate cravings but to understand them, honor the needs they represent, and gradually expand our ways of meeting those needs.
A platform for social impact that addresses both individual and collective trauma creates conditions where healing becomes possible not just for one person but for entire communities struggling with the legacy of unhealed wounds.
Want to take the next step to decode your cravings and heal the gut-brain connection that trauma disrupted? Join AlignUs to access trauma-informed nutrition guidance, nervous system regulation tools, and a community that understands the journey from surviving to thriving.
Because your cravings aren’t character flaws – they’re invitations to deeper healing.